As Beaufort Co. breaks COVID-19 case records, how are hospitals faring with omicron?
READ MORE
COVID-19 in the Lowcountry
Here’s the latest on the omicron variant surge, COVID-19 guidance and more in the Lowcountry.
Expand All
Beaufort County’s wave of omicron infections has not inundated local hospitals with admitted coronavirus patients, according to promising new data from the medical centers.
The Island Packet and Beaufort Gazette late last week reported that county hospitals were stressed by a recent spike in demand for COVID-19 testing and treatment at outpatient clinics and emergency rooms, but the number of seriously ill coronavirus patients had not jumped to the levels last seen during the 2021 delta surge.
(The newspapers’ report was based on hospital data current as of Jan. 4 and Jan. 5.)
Roughly a week later, the hospitals’ inpatient numbers have not dramatically changed, which is good news for the Lowcountry, where 317 newly confirmed infections are now being logged each day in Beaufort County, on average — a new record.
Beaufort Memorial Hospital, as of late Monday, was treating 12 coronavirus inpatients, with one of those people in the intensive care unit. None was on a ventilator, according to spokeswoman Dee Robinson.
For context: The hospital on Jan. 4 had 15 COVID-19 inpatients, with one of those people in the ICU, CEO Russell Baxley said at the time. At one point in mid-September, during the delta surge, the hospital had 60 coronavirus inpatients.
Hilton Head Regional Healthcare, meanwhile, was treating 15 coronavirus inpatients as of Tuesday, spokeswoman Valerie Burrow said.
The health care system, which includes Hilton Head and Coastal Carolina hospitals, had 12 COVID-19 inpatients on Jan. 5.
Burrow said there were three coronavirus inpatients in ICU beds at Hilton Head Regional Healthcare on both Tuesday and Jan. 5.
Omicron seems to be extremely transmissible, but not as virulent as delta, said Carlye Gilbert, the health care system’s infection preventionist, in a previous interview.
“It’s a sore throat and sinus pressure,” Gilbert said of local coronavirus symptoms, “then it becomes weakness, even altered mental status, where people are just profoundly weak and they’re not acting like themselves.”
Beaufort County last Saturday reported a record-breaking single-day high of 543 newly confirmed COVID-19 cases.
The national picture
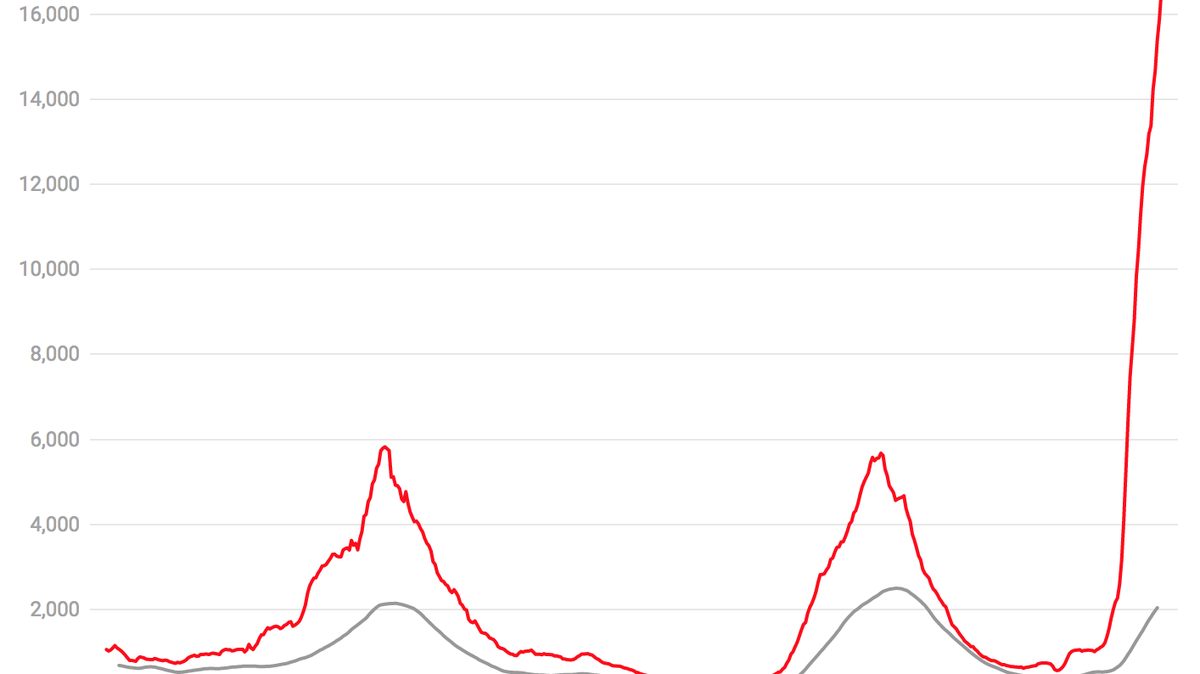
The United States has more people hospitalized with COVID-19 now than ever before.
There were 155,935 coronavirus inpatients nationwide as of Thursday, according to the U.S. Department of Health and Human Services.
That could spell trouble for South Carolina, given that the northeastern states that currently have some of the country’s highest hospitalization rates, such as New York and New Jersey, were hit by omicron earlier than the Palmetto State was.
Hospitalizations typically lag behind coronavirus infections by about two weeks, meaning the worst could still be in store for South Carolina, which has a lower vaccination rate than states in the Northeast. (Beaufort County’s omicron surge kicked into high gear on Dec. 31, which was roughly two weeks ago.)
On the other hand, both locally and nationally, hospital officials have recently said that omicron seems to produce milder disease than delta, which leaves open the possibility that Beaufort County will be spared from an influx of COVID-19 inpatients.
Gilbert, for example, last week said that patients have not been presenting with COVID-19 pneumonia.
Baxley added that hospitalized coronavirus patients are now being admitted for shorter lengths of time at Beaufort Memorial Hospital, spending an average of roughly three to four days at the medical center instead of seven to eight days, which was typical last year as delta swept across the Lowcountry.
One recent study, meanwhile, found that among nearly 70,000 patients with omicron or delta infections in the Kaiser Permanente Southern California health care system, zero people with omicron needed mechanical ventilation, while 11 people with delta did.
There’s also been an increase in the rate of “incidental” coronavirus inpatients at some hospitals, according to The New York Times. Those are people who test positive for COVID-19 after being admitted to a medical center “primarily” because of another ailment.
The Jackson Health System in Florida on Jan. 4 reported that 249, or about 53%, of its 471 COVID-19 inpatients were incidentally found to be positive.

Incidental patient data
The S.C. Department of Health and Environmental Control does not publish statewide data on incidental COVID-19 patients.
And Dr. Brannon Traxler, the state’s director of public health, told The Island Packet and Beaufort Gazette on Wednesday that DHEC has no plans to start tracking such data.
Why?
Hospitals, Traxler said, already report patient counts and other facility-level data to government officials.
“To do an even more detailed breakdown would take even more of the hospital resources and time and staffing to report,” Traxler said.
HHS does not require U.S. hospitals to send incidental patient data to federal health authorities. If that guidance were to change, statewide data on such hospitalizations might become available.
“I don’t know if the federal government has any plans to change it,” Traxler said, “but at this time, you’re really only going to find the health care system-level data.”
HHS did not immediately respond to a request for comment Thursday.
This story was originally published January 13, 2022 at 2:44 PM.