‘Totally ridiculous:’ You may pay more to visit these hospitals in Beaufort, Jasper counties
READ MORE
Health care costs in Beaufort County
Read more in the series about health care costs in Beaufort County.
Expand All
.jpeg)
‘Totally ridiculous:’ You may pay more to visit these hospitals in Beaufort, Jasper counties
Is an increase in concierge doctors causing a ‘wealth care’ problem on Hilton Head?

Hilton Head doctors charge more than Charleston, Columbia for some services, data show

Hilton Head residents concerned about lack of doctors, specialists. Here’s what officials are doing
Luke Drager, 15, and his family were vacationing on Hilton Head from Westminster, Maryland when he “wiped out” while skim-boarding on the beach.
Fearing that his foot or ankle was broken, his parents, Beth and Ron Drager, rushed him to Hilton Head Hospital’s emergency room. The family got an estimate of $768.95 before any X-rays were taken.
Luckily, nothing was broken. But four months later, a $2,498.09 bill arrived in the mail from Hilton Head Hospital — $1,612 for emergency room care on top of the cost of X-rays.
“I was shocked,” Ron Drager said.“I was expecting (the bill) to be much closer to the estimate. That’s the highest charge I’ve ever had for an ER bill ... and it was for three X-rays.”
His family unsuccessfully fought the hospital over the bill, Ron Drager said. Hospital representatives told the family the estimate was only for the X-rays, according to Ron Drager.
The family’s complaints are not unique. Hilton Head Hospital and Coastal Carolina Hospital charge more than Beaufort Memorial for many of the same services, according to a review of published charges by The Island Packet and The Beaufort Gazette.
The newspapers compared hospital charges for what the South Carolina Hospital Association lists as the top 10 reasons for hospitalizations in the state — including child birth, pneumonia and heart failure.
Specifically, the newspapers found:
- Hilton Head and Coastal Carolina hospitals — both owned by Hilton Head Regional Healthcare — charge between 11 percent and nearly 84 percent more for a variety of treatments, ranging from knee replacements to heart failure.
- The two hospitals are also significantly more expensive for expectant mothers than Beaufort Memorial, a nonprofit hospital. The average listed charges for Hilton Head and Coastal Carolina hospitals for a vaginal delivery is nearly 115 percent more than the average listed cost at Beaufort Memorial. For a Cesarean section, that gap grows to 354 percent.
The charges are published by the hospitals and likely do not reflect the amount a patient actually pays. Private insurance, Medicare or Medicaid would pick up part of the tab in many cases. Other factors also affect the final price.
Hilton Head leaders look to address health care
Area leaders say they’ve heard residents’ cost complaints and are working to determine what’s behind them.
Bill Harkins, Hilton Head’s mayor pro tem and a former senior health care CEO with 35 years of experience, speculates that the town’s higher cost of living — which lends itself to higher costs to run health care facilities — could be a culprit.
So could the relatively low volume of patients compared to nearby hospitals. Beaufort Memorial has 197 beds, according to a spokeswoman, while Hilton Head Hospital has 93 and Coastal Carolina has 41, according to their websites.
Harkins said he is forming a “health care think tank” this year to address what he says is a problem with health care, doctor shortages and high medical costs on the island where the median age is 50.9 years old, according to 2010 census data.
In Beaufort County, the population ranges from low-income families to affluent retirees and everyone in between, which may also help explain price variations.
“(The) older population is going to be more expensive to care for,” said Lindsey Woodworth, a professor of economics at the University of South Carolina, especially in “areas with a primary care shortage.”
She said “doctors are just as susceptible” to labor costs such as housing, transportation and other factors of cost of living — which has been proven to to vary greatly across Beaufort County.
Mayor John McCann, who said he supports Harkins’ effort to bring more medical services to the island and announced the think tank group at the December Town Council workshop, told The Island Packet in September that town leaders were “missing the boat on health care.”
.png)
Unequal costs for equal treatment?
Ron Peduzzi of Hilton Head Island had a kidney stone attack last spring.
It was 6:30 a.m. and Peduzzi was eating a bowl of cereal when he felt severe pressure in his back that was like “being in the jaws of a tiger.”
“I was like, ‘Oh boy, I know what this is,’” he said.
With no doctors’ offices open on Hilton Head yet, Peduzzi went straight to the ER at Hilton Head Hospital.
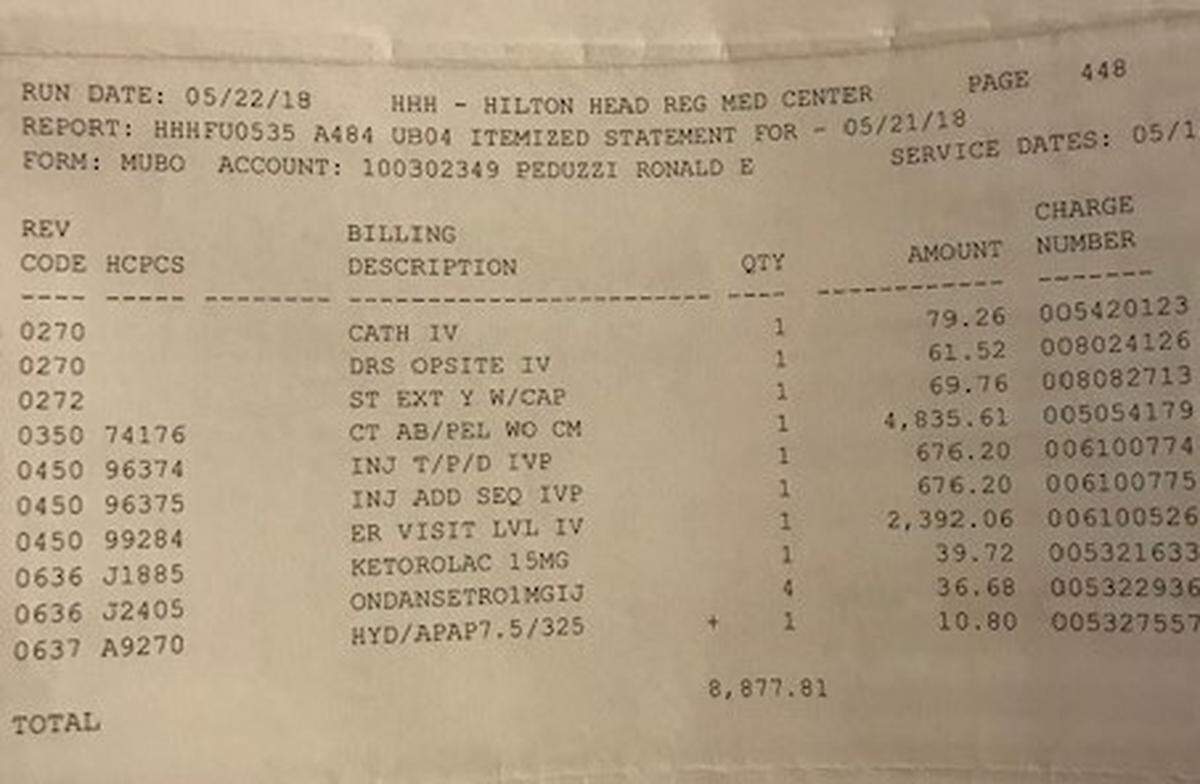
Weeks later he got the bill, which totaled $8,877.81.
“I just find it totally ridiculous,” he said, adding that it was double the cost of an emergency room visit in Pennsylvania when he experienced a similar attack years ago.
What’s causing the huge range in hospital charges?
No one can say for sure.
According to the South Carolina Hospital Association, charges can vary between hospitals because of debt incurred by updating facilities or making big purchases, the number of people on staff and whether the hospital is in an area experiencing a health care workforce shortage.
Daisy Burroughs, the public relations manager for Hilton Head Hospital, would not comment specifically on why the island’s only hospital often charges more, but wrote in a statement that prices “can be affected by capital investments for new technology, equipment and services, the intensity of care provided, staffing costs and the taxes paid on supplies purchased.”
Russell Baxley, CEO of Beaufort Memorial said in a statement his hospital has kept charges “fairly consistent year after year,” which may be why its prices are lower than the other two hospitals.
“Every organization and/or system has its own approach to determining charges,” Baxley wrote. “Charges often differ as each organization analyzes its costs for providing services and chooses to implement increases to charges if they feel they are warranted.”
Just why costs vary so much around the nation is the “million dollar question,” according to Louise Norris, a health policy analyst who writes for healthinsurance.org, Verywell and owns a Colorado health insurance brokerage company with her husband.
“The rates are always a negotiating process,” Norris said. “The provider will say, ‘How about you pay me this much?’ and the insurance will say ‘Nope, how about this?’”
What Medicare, or other government health care, will pay, however, does not fluctuate as much because they are federal programs.
“The negotiated rates are always going to be lower with Medicare than with private insurance,” Norris said.
The amount a patient pays also has to do with whether the doctor they saw was in-network and whether they have a deductible, a copayment or coinsurance. Once those have been paid, the patient may still be “balance billed,” or, billed the remaining cost, in some situations.
Hospital upgrades also affect pricing, said Robert Hartwig, an associate professor of finance at the University of South Carolina.
“Some institutions very actively market themselves as having high quality staff, childbirth care... or luxury suites for those who can afford it,” Hartwig said, noting those choice features can raise the price tag. “Price might be part of it, but part of it is going to be the experience of (the visit).”

Four stitches that cost $1,200?
Heather Nolte was cutting brussels sprouts on Thanksgiving when she sliced her pinky finger with a knife.
Two hours and four stitches later, she was bandaged and back from Hilton Head Hospital in time for a slightly delayed feast.
Nolte, 43, was also stuck with a $930.24 ER bill and an additional $300 bill from a doctor’s office.
Nolte lives in the city of Torreón in Coahuila, Mexico and was on Hilton Head visiting family.
She said her Mexican insurance will reimburse her for the incident, but “it really would have been cheaper for me to fly back to Mexico, have it fixed and fly back to South Carolina versus going to an American hospital. If I had done this here (in Mexico), there is a service that would come to my house and stitch my finger there.”
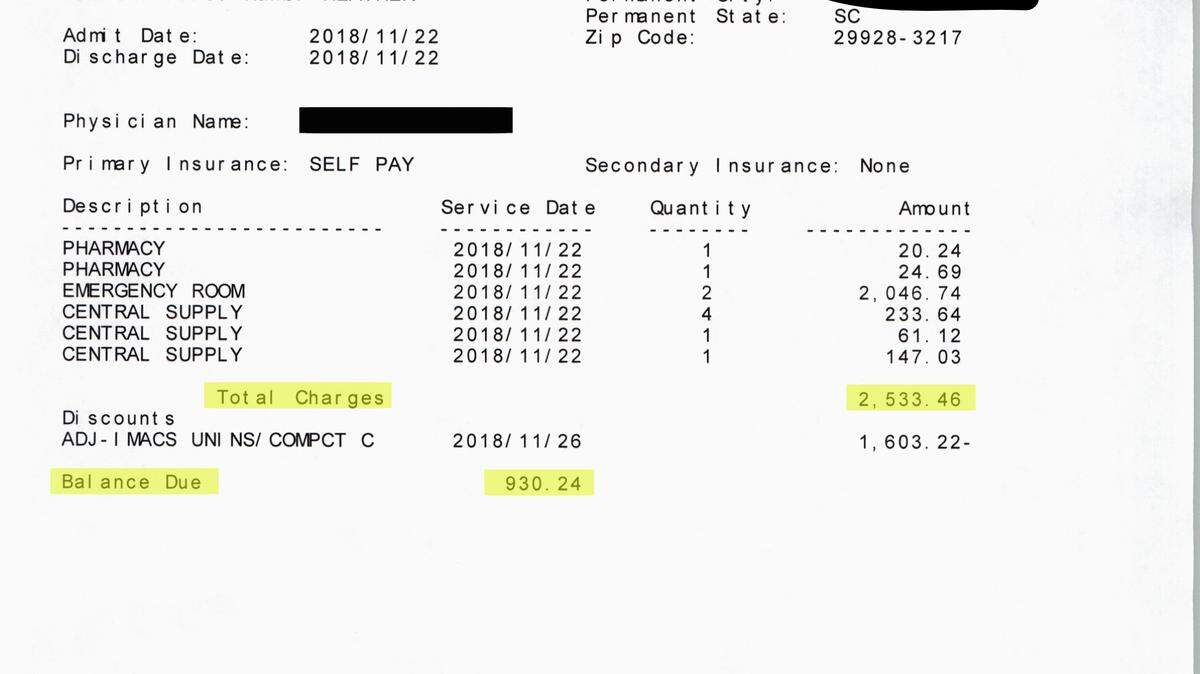
Though a pinky needing stitches is not a listed procedure, an emergency room visit for a “superficial injury” will also run someone a few hundred dollars more at Hilton Head Hospital compared to the other two, according to the median charge.
So what’s a would-be patient to do to make sure they’re getting the best price?
Options are limited, and efforts to increase transparency have fallen short.
For example, an online tool launched by the Trump Administration on Jan. 1 that allows patients to view hospitals’ “charge sheets” doesn’t allow for true price comparisons.
That’s because hospitals can mark charges up to 200 percent to get insurance companies to start bargaining at a higher price, said Lindsey Woodworth, a professor of economics at the University of South Carolina.
So listed prices don’t align with the amount patients ultimately pay.
“The intention of (publishing charges) is good,” Woodworth said. “But the numbers it’s showing you don’t mean a whole lot.”
What’s the data?
This story was originally published February 8, 2019 at 5:00 AM.