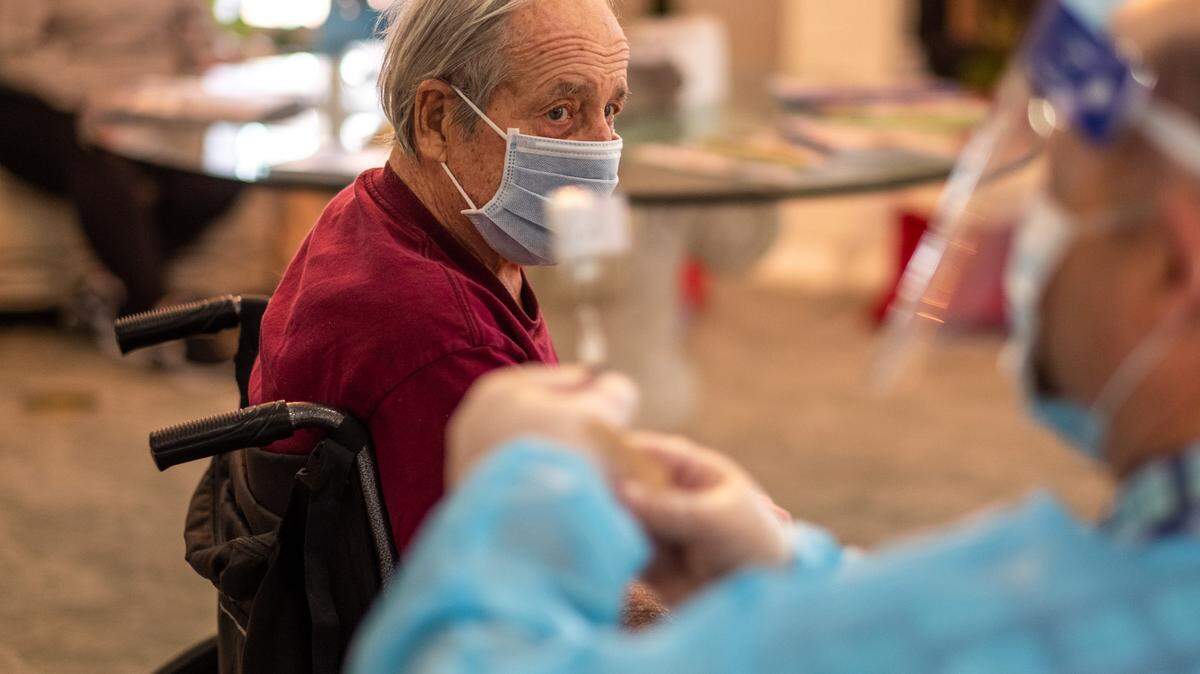
School COVID policies are ‘doing the opposite’ of keeping kids safe, SC pediatrician says
READ MORE
COVID-19 spikes again in South Carolina
Here’s the latest on the omicron variant surge, COVID-19 guidance and more in South Carolina.
Expand All
The highly contagious delta variant has sent COVID-19 cases soaring in South Carolina over the last six weeks, turning the state into one of the nation’s foremost coronavirus hotspots.
No age group has seen a larger recent spike in cases than children, who account for roughly 30% of new cases. The increase likely stems from the fact that most are unvaccinated (only 34% of South Carolinians age 12-19 have gotten a single shot), or are not yet eligible to get vaccinated.
The reopening of schools in recent weeks, where masks are now optional and social distancing is made difficult by larger class sizes, has contributed to the explosion of COVID cases, especially among young children.
Thousands of children have contracted COVID-19 in just the first few weeks of the fall semester and thousands more are out of school quarantining due to COVID exposure. Dozens of schools have had to close their doors and return to remote learning because of coronavirus outbreaks.
The State spoke with Dr. Deborah Greenhouse, a Columbia pediatrician and past president of the South Carolina chapter of the American Academy of Pediatrics to better understand how COVID-19 affects children and what parents can do.
Q: Are the symptoms of COVID-19 in children the same as in adults?
A: In a lot of cases, they are very similar. You can see cough, congestion, runny nose, fever, headache, upset stomach. Almost anything can be a symptom of COVID-19 in a child.
What you don’t tend to see as much early on in the disease in children is the respiratory distress. That’s not to say it can’t happen, and unfortunately, in some cases it does. And we do have children that end up in the hospital with respiratory distress from COVID-19, we do have children who end up in the intensive care unit, we do have children who end up on ventilators, and we have several in South Carolina right now.
Babies with COVID-19, obviously it’s trickier. They can’t tell you what they’re feeling. So it may just be the baby that’s fussier than usual. It may be the baby with a fever and you can’t tell why.
Q: Are children at greater risk from the delta variant than other strains of COVID-19?
A: The biggest risk that we absolutely know to be true of the delta variant is simply the fact that it is so much more contagious and easily spread than the initial strain of coronavirus.
What that means is that we are seeing far, far, far more children being exposed to coronavirus, especially now that our schools are open, and especially now that in South Carolina our schools are open without mask mandates.
Whether the delta variant is actually making the kids sicker is still a little bit up in the air. My gut instinct is that it is, that it is causing more severe illness as well. But unfortunately, we’re only going to be able to really say that in retrospect, when we’re able to look back and see what proportion of kids with coronavirus are actually getting very sick and ending up in the hospital.
Q: Are infants at greater risk of developing severe COVID illness because their immune systems are not as developed as older children?
A: I have seen a couple of new babies now that got it from their mom right at the time of delivery or just before the time of delivery. Those babies that I have seen and similar babies that my partners have seen have done well thus far. So we have not seen anything yet that would make me think that new infants are more vulnerable than older kids. It actually seems, if anything, that the kids we’re seeing that end up in the intensive care unit largely tend to be the older kids.
Q: What is the typical course of illness in children who catch COVID-19? Are most children asymptomatic or mildly symptomatic, and how often do children get severely ill?
A: The majority of young children with COVID will do well. The majority will have a flu-like illness, will recover, will do well, hopefully without long-lasting side effects.
Part of the problem here is that we don’t honestly know what are the long-term complications of the delta variant. We do know that some kids do develop long-haul COVID, just like adults can. We do know that is a thing at this point and that’s a little bit scary when you look at the incredibly high number of kids who are now catching it.
The risk factors that seem to exist for adults, some of those same risk factors seem to exist for children. Obesity does appear to be a risk factor for a severe course of COVID. Other chronic illnesses. Autism seems to have a negative effect on the course of COVID as well. Down syndrome may as well.

Q: What is MIS-C and how common is it?
A: MIS-C is multisystem inflammatory syndrome in children, and essentially it is exactly that. It’s an inflammatory disorder that develops usually several weeks after a child has had COVID, sometimes who didn’t know they had COVID, which can make it a trickier diagnosis.
But it involves multiple systems. It can involve fever for a prolonged period of time, longer than five days. Rashes, joint problems, red eyes, red lips, lymph node swelling. It can look a lot like another inflammatory disorder that pediatricians are used to seeing called Kawasaki syndrome. But there are some things that set it aside. The type of heart inflammation you get with MIS-C is a little bit different than what you typically see with Kawasaki.
Again, most kids with MIS-C over time will do well, but they require hospitalization, they require sometimes a very intensive treatment in the intensive care unit. Usually the kids with MIS-C are not infants, they tend to be a little bit older.
Q: Are MIS-C cases predicted by the severity of COVID illness or other COVID risk factors?
A: We really don’t know what triggers it, much like, honestly, we don’t know for sure what triggers Kawasaki syndrome. Some of the kids who develop MIS-C did not have a diagnosed case of COVID preceding it, but if you do tests looking at antibodies and other things looking to see, hey, did they have it? Sometimes you will identify it after the fact.
Q: Do children receive the same treatment for COVID-19 as adults?
A: Your typical child with COVID-19 with just mild illness is generally just going to be treated symptomatically, and that’s going to be Tylenol or Ibuprofen for their fever, lots of fluids, lots of rest.
Monoclonal antibodies absolutely are approved for children above 12 years of age and above 40 kilograms in weight (roughly 88 pounds) who have a risk factor for severe outcome of COVID-19. And there are a bunch of risk factors. Probably the one that we see the most is kids that are overweight.
But you want to give monoclonal antibodies early. If they get to the point where they need to be in the hospital on oxygen then they don’t qualify for monoclonal antibodies. It’s really more of a prophylactic thing.
Other than that it is largely symptomatic, and if the kids get into respiratory trouble the treatment, just like in adults, is going to be oxygen. And then if the oxygen doesn’t work then you’re looking at oxygen with pressure, like BiPap (bilevel positive airway pressure), typically. And then if those kinds of things don’t work, then you’re looking at ventilators and things that you really don’t want to be doing.
Q: What accounts for the increase in COVID-19 outbreaks in school this year?
A: We basically created the perfect storm this year, unfortunately.
Last year, we used all of the precautions we had at our disposal. We initially started our schools virtually and when it was safe to do so, the kids went back into school, but in a hybrid fashion, so you had smaller groups of kids in the school. They were wearing masks, almost uniformly. Because they were able to distance, you didn’t have the kids right on top of one another and you didn’t have the delta variant. And then as you got later into the school year, you started having folks getting vaccinated.
This year, all of those mitigation strategies and all of those layered protections are gone. So, you have classrooms that are chock full of kids, you have a ban on mask mandates, so you have some kids wearing masks but you don’t have everyone wearing masks, you don’t have everyone vaccinated, and certainly kids under 12 can’t be vaccinated. In a lot of places you have old schools with poor ventilation and you have a variant of the virus that is much more contagious.
Q: What do you tell parents who ask your advice about sending their children to school, if virtual learning is an option?
A: Unfortunately, virtual is not an option for most of them because rules were put in place this year that prevent more than a certain percentage of kids from being allowed to participate in virtual learning.
Some parents have simply pulled their kids out and are just home schooling them. I have several families that have done that at this point and they’re very happy with that decision. Some families chose to go to private schools this year because some of the private schools were using better preventative strategies and were enforcing mask mandates.
But obviously, that involves a level of privilege that the vast majority of folks in South Carolina do not have. So most families were stuck. Most of the families were stuck sending their kids to school in a situation that they know is not safe and, in a lot of cases, unfortunately, it didn’t play out well and a lot of folks sent their kids to school and found their kids quarantined back at home within a week.
Q: Would you send your own children to school at this point?
A: If I had children that were too young to be vaccinated, at this stage in the game, honestly, they probably would be attending the Cutler Jewish Day School this year. A small, private school that had a mask mandate in place. Now that school is also, like every other school, they’re having their own struggles this year. Every school is. But that probably is a decision that I would have made.
As I said, that involves a level of privilege that most folks don’t have. But I’m not going to lie, I suspect that is the decision I would have made. Would I have chosen to send my kids to a large, public school without a mask mandate knowing the classes would be full, the ventilation would not be very good? No. I could not have done that in good conscience.
As a community, as a state, we should be doing everything in our power to keep our children safe. Not only are we not doing that, in many ways, we’re doing the opposite. And that’s simply not OK.
Q: How much caution should parents exercise with a child who is too young to get vaccinated?
A: I really think given the incredible level of community spread that we have right now, and given what I am seeing in my office, I would advise families with kids too young to be vaccinated to really be minimizing the interaction that they are having.
Interactions with other kids or with unvaccinated older kids and adults, it should be outdoors if they can. It should be distanced if they can. So letting the kids play in the park is going to be infinitely better than having them play in someone’s house in a playroom.
I absolutely would not be taking my unvaccinated young children to eat indoors in a restaurant right now. I just wouldn’t do it. Shoot, I’m not going to eat indoors in a restaurant right now. If I had to take them to the grocery store, I would absolutely have them wearing a mask. If I didn’t have to take them to the grocery store, I simply wouldn’t right now.
I think we really need to be trying to protect our young kids. We don’t know what the long-term ramifications of COVID might be.
Q: What do you tell parents who are hesitant to vaccinate their child?
A: What I try and do in that scenario is talk to the parents about comparing the risks of the disease and thinking about what is the risk to my child if they catch COVID versus the perceived risks of the vaccine. And then benefits of the vaccine versus benefits of the disease, of which there aren’t any.
And if you really do those comparisons, I think it becomes a very, very easy decision to vaccinate kids above 12. The data is there, the data is solid. Millions of folks have been vaccinated at this point.
The other thing I point out is that if you look at the folks that are in the hospital, in the ICU and on ventilators, the vast, vast majority are unvaccinated. Looking at the numbers from our children’s hospital, they’re all unvaccinated right now. And most of them were old enough to get the vaccine.
So that in my book is the best argument for the vaccine. It’s not 100% effective at preventing all COVID. No vaccine is 100% effective at preventing illness. I mean that just doesn’t exist. But it is extremely effective at preventing severe illness, preventing hospitalization, preventing admission to the ICU and preventing death.
Editor’s Note: The interview has been condensed for length and clarity.
This story was originally published September 3, 2021 at 10:39 AM with the headline "School COVID policies are ‘doing the opposite’ of keeping kids safe, SC pediatrician says."













%20(5).jpeg)